by Preventx
Mark Clune,1 Tony Proom,2 Jane Hosking,1 Steve Bonner3 and John White1
1 Preventx, 2East Sussex County Council, 3East Sussex Healthcare Trust
Background
Online Postal Self Sampling (OPSS) services have become the default asymptomatic STI testing option in many areas of England. This has led to concerns that OPSS may only be accessible by users who are not digitally excluded, and that a ‘digital divide’ could be contributing to a widening of sexual health inequalities. OPSS services collect ethnicity and demographic data that allows Index of Multiple Deprivation Decile (IMDD) to be identified.
Methods
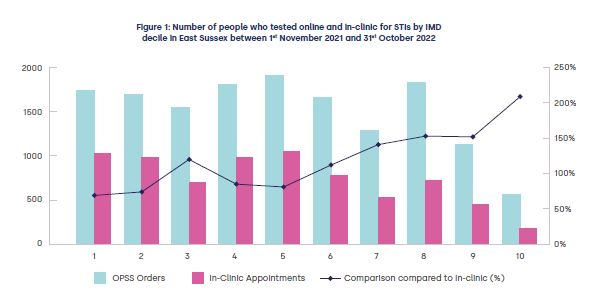
We conducted a retrospective analysis of all 15,174 OPSS orders and 7526 in-clinic testing appointments between November 1st 2021 and October 31st 2022 in East Sussex, England. We compared the number of OPSS orders and clinic appointments for testing by ethnicity and IMDD*. *IMDD is used to assess relative deprivation: lower deciles (1) have the poorest health outcomes and higher deciles (10) have better health outcomes.
Results
Twice as many individuals used OPSS testing compared to in-clinic testing appointments (n=15174 vs. 7526). For IMDD, the ratio of OPSS:clinic testing varied from 1.69 in the most deprived areas to 3.09 in the least deprived areas. For ethnicity, 87% of the total population identified as White British, among whom the OPSS: clinic testing ratio was 2.16. For those ethnicities with higher UK STI prevalence, OPSS testing rates were 2.1 to 5.2 times higher than clinic testing episodes.
Conclusion
Higher numbers of OPSS testing episodes occurred across all IMDD deciles as well as most higher STI risk ethnicities compared to in-clinic testing. OPSS in this region is declined if significant STI symptoms are present or safeguarding triggers disclosed in those aged <18 years. As higher STI prevalence is seen in lower IMDD and Black African/Caribbean/Mixed ethnicities this might underestimate intended OPSS use among those risk groups as they would be diverted to clinic for assessment. These data suggest that OPSS testing is accessed by those across all deprivation deciles and among ethnicities with the poorest sexual health outcomes and we are unable to discern clear evidence of a digital divide in this population. OPSS could contribute to the reduction in sexual health inequalities but more research is needed in other populations to explore if these results are replicated.
About the author:
Claire is the Senior Digital Marketing Executive at Preventx.